Introduction
Eye Health and Autoimmune Diseases are deeply connected, and many autoimmune conditions can directly damage your eyes without early warning signs. Autoimmune diseases attack the body’s own tissues — and the eyes are among the most vulnerable.
From dryness and inflammation to retinal damage and even vision loss, eye complications are extremely common in autoimmune conditions like:
- Rheumatoid Arthritis (RA)
- Lupus (SLE)
- Sjögren’s Syndrome
- Psoriasis
- Multiple Sclerosis (MS)
- Thyroid Eye Disease (Graves)
- Inflammatory Bowel Disease (Crohn’s & Ulcerative Colitis)
- Ankylosing Spondylitis
- Vasculitis
- Type 1 Diabetes
Because autoimmune reactions involve chronic inflammation, your eyes end up being one of the first organs to show symptoms — often before systemic problems appear.
In this comprehensive guide, you’ll learn:
- Which autoimmune diseases affect your eyes most
- Early eye symptoms you should never ignore
- How inflammation damages ocular structures
- What tests diagnose autoimmune-related eye disease
- The best medical and natural treatments
- Long-term protection strategies backed by ophthalmologists
1. How Autoimmune Diseases Affect Eye Health
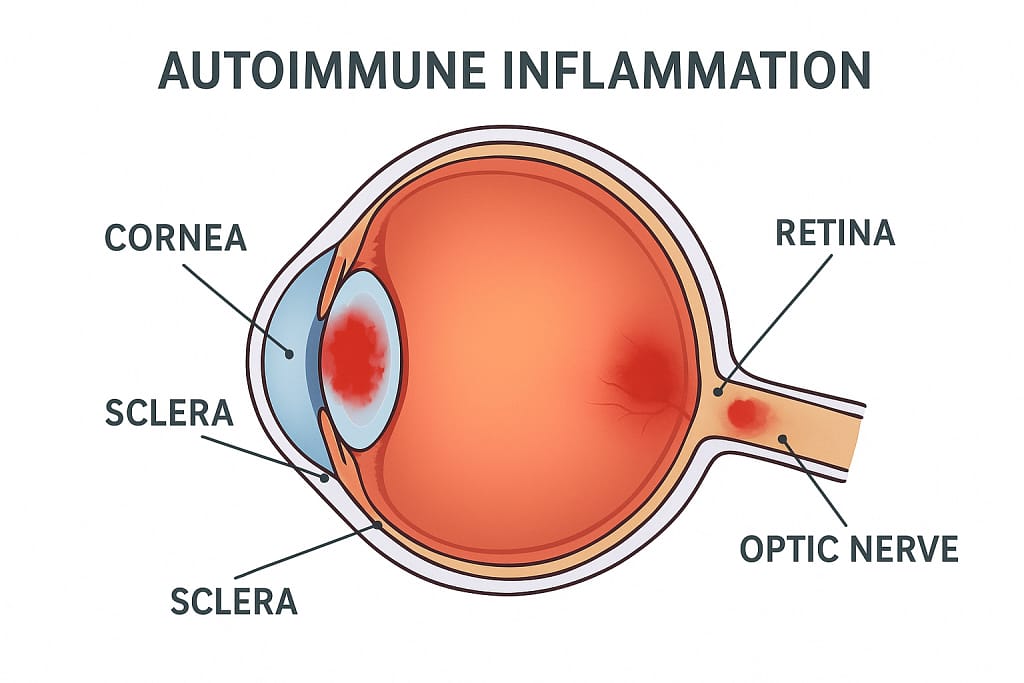
Autoimmune reactions trigger inflammation throughout the body, including the:
- tear glands (dry eye)
- sclera (scleritis)
- cornea (keratitis)
- retina (vasculitis, macular edema)
- optic nerve (neuritis)
This inflammation can be:
✔ Surface inflammation
• Dry eye
• Blepharitis
• Corneal erosions
✔ Middle-layer inflammation
• Uveitis
• Scleritis
• Episcleritis
✔ Deep eye or nerve damage
• Optic neuritis
• Retinal vasculitis
• Macular edema
Autoimmune eye issues often follow cycles:
flare → remission → flare
The earlier they are treated, the better the long-term prognosis.
2. Autoimmune Diseases Most Commonly Affecting the Eyes
Below is the list of autoimmune conditions most associated with eye symptoms — with detailed explanations for each.
Rheumatoid Arthritis (RA)
RA frequently causes:
- Dry Eye (most common)
- Blepharitis
- Scleritis (very painful, dangerous)
- Uveitis
- Peripheral ulcerative keratitis
RA-related scleritis is especially serious — untreated, it can lead to perforation.
Sjögren’s Syndrome
The #1 autoimmune cause of severe dry eye.
Sjögren’s attacks the lacrimal glands → tear production decreases → cornea becomes vulnerable.
Common complications:
- severe dryness
- burning pain
- blurred vision
- recurrent infections
- corneal erosions
Lupus (SLE)
Triggers multi-layer eye inflammation:
- Retinal vasculitis
- Optic neuropathy
- Dry eye
- Photophobia
- Conjunctival inflammation
Retinal vasculitis can cause permanent vision loss.
Psoriasis & Psoriatic Arthritis
Often leads to:
- Uveitis
- Dry eyes
- Conjunctivitis
- Meibomian gland dysfunction (MGD)
Ankylosing Spondylitis (AS)
30–40% of AS patients develop recurrent uveitis.
It can cause:
- eye pain
- light sensitivity
- sudden blurry vision
Thyroid Eye Disease (Graves’)
Symptoms include:
- bulging eyes
- dryness
- corneal exposure
- double vision
Multiple Sclerosis (MS)
Most common symptom: optic neuritis, causing:
- sudden vision loss
- pain with eye movement
- color desaturation
IBD (Crohn’s & Ulcerative Colitis)
Common ocular issues:
- episcleritis
- scleritis
- uveitis
- dry eye
- corneal inflammation
3. Early Warning Signs: Symptoms You Should Never Ignore
Autoimmune eye symptoms can start mild but develop fast.
Seek urgent care if you experience:
Common symptoms
- dryness
- burning or gritty sensation
- redness
- light sensitivity
Serious symptoms
- eye pain that worsens with movement
- blurry or dim vision
- halos around lights
- sudden floaters or flashes
- blind spots
- distorted vision
- double vision
- loss of contrast
💡 Did You Know?
More than 50% of autoimmune patients develop eye symptoms — but only 25% report them early.
Early diagnosis prevents irreversible vision loss.
Related Posts
4. How Inflammation Damages the Eyes
Autoimmune inflammation is powerful. Here’s how it destroys ocular tissues:
A) Tear Gland Damage (Dry Eye)
Inflammation shrinks the lacrimal glands → less tears → unstable tear film → corneal damage.
Common in:
✔ RA
✔ Sjögren’s
✔ Lupus
B) Meibomian Gland Dysfunction (MGD)
Inflamed oil glands produce thick meibum → quick tear evaporation → severe dryness.
C) Scleritis
A painful condition where the white of the eye becomes deeply inflamed.
If untreated → can lead to vision loss.
Inflammation of the uvea; can damage:
- retina
- macula
- optic nerve
Uveitis is an emergency.
E) Optic Neuritis
Common in MS and lupus.
Damages the optic nerve → sudden vision loss.
5. Diagnosis: How Doctors Identify Autoimmune Eye Disease
You may undergo:
✔ Eye Exam
Visual acuity, slit-lamp exam, retinal check.
✔ Schirmer Test
Measures tear production.
✔ Meibography
Shows damaged meibomian glands.
✔ OCT
Detects retinal swelling and optic nerve issues.
✔ Blood Tests
ANA, RF, anti-SSA, anti-dsDNA, HLA-B27.
✔ Imaging
MRI (MS-related optic neuritis).
Autoimmune eye complications are one of the leading causes of preventable vision loss — early detection improves outcomes by up to 80%.
6. Treatment Options
The ideal treatment depends on the autoimmune condition and eye complication.
A) Artificial Tears & Gels
For dryness and corneal irritation.
B) Anti-Inflammatory Eye Drops
- corticosteroids
- cyclosporine (Restasis)
- lifitegrast (Xiidra)
C) Warm Compresses for MGD
Softens meibum and improves tear quality.
D) Oral Medications
DMARDs (methotrexate)
Biologics (Humira, Enbrel)
Steroids
NSAIDs
E) Punctal Plugs
Retain tears.
F) Surgery (rare)
For severe corneal damage or thyroid eye disease.

7. Long-Term Eye Protection Strategies
✔ Control systemic inflammation
Take prescribed autoimmune medications.
✔ Use preservative-free tears
Less irritation.
✔ Maintain vitamin D levels
Reduces inflammation.
✔ Omega-3 supplements
Improve tear film quality.
✔ Wear sunglasses
Blocks UV and reduces flares.
✔ Avoid smoking and dry environments
✔ Regular eye exams
Every 3–6 months.
8. Diet for Autoimmune Eye Protection
Focus on anti-inflammatory nutrients:
- Omega-3 (salmon, sardines, flaxseed oil)
- Vitamin A (carrots, sweet potato)
- Lutein & zeaxanthin (spinach, kale)
- Curcumin
- Vitamin D
Avoid:
- sugar
- processed foods
- seed oils
- alcohol excess
9. When to See a Doctor Immediately
If you experience:
- sudden pain
- sudden vision loss
- flashes / floaters
- severe redness
- double vision
- halos
- dim or “greyed” vision
These can indicate emergencies like:
- retinal tear
- optic neuritis
- scleritis
- severe uveitis
For expert-reviewed clinical guidelines on autoimmune eye complications, visit the American Academy of Ophthalmology (AAO).
FAQ – Eye Health & Autoimmune Diseases
1. Can autoimmune diseases permanently damage vision?
Yes. Conditions like lupus, RA, or MS can cause retinal damage, optic neuritis, or severe dry eye leading to corneal injury.
2. What is the most common autoimmune eye symptom?
Dry eye is the most widespread symptom across nearly all autoimmune disorders.
3. Can eye flare-ups predict systemic flares?
In some diseases like lupus and RA — yes, eye inflammation can signal a larger autoimmune flare.
4. Are autoimmune eye diseases curable?
They are manageable but not fully curable — early treatment is essential.
5. How often should autoimmune patients see an eye doctor?
Every 3–6 months, or immediately if new symptoms appear.
14. Key Takeaway
Autoimmune diseases and eye health are deeply connected.
Inflammation can affect nearly every structure of the eye — from tear glands to the optic nerve.
Early detection and coordinated care between:
- rheumatologists
- ophthalmologists
- immunologists
…is the best way to protect long-term vision.
A Note from the Founder
"I started CVT because eye health is personal to me. After losing sight in my left eye due to a childhood injury and managing high intraocular pressure for decades, I’ve dedicated my life to finding the best ways to protect the vision we have. Every piece of advice on this site is researched with that same level of care and responsibility. Thank you for being here."