Introduction
Ocular migraines causes symptoms that can be both frightening and confusing, often appearing as sudden flashes of light or zig-zag patterns across your field of vision. While these neurological events are usually temporary, understanding the link between triggers and visual disturbances is essential for effective prevention Migraines are well-known for their intense headaches, but not all migraines are the same. Some affect vision more than the head. Ocular migraines, also called visual migraines or retinal migraines, are a special type that can cause sudden vision disturbances such as flashing lights, zig-zag patterns, or temporary vision loss in one eye.
While they usually resolve on their own within 20–30 minutes, they can be alarming and may signal an underlying condition. In this article, we will explore what ocular migraines are, their causes, triggers, prevention strategies, and treatment options.While these episodes usually resolve within 30 minutes, they can be alarming signs of how our brain and eyes interact. Understanding ocular migraines causes symptoms is the first step toward prevention; for a complete guide on maintaining your sight, visit our Eye Health Basics HUB.
What Are Ocular Migraines?
- Definition: neurological event, not an eye disease.
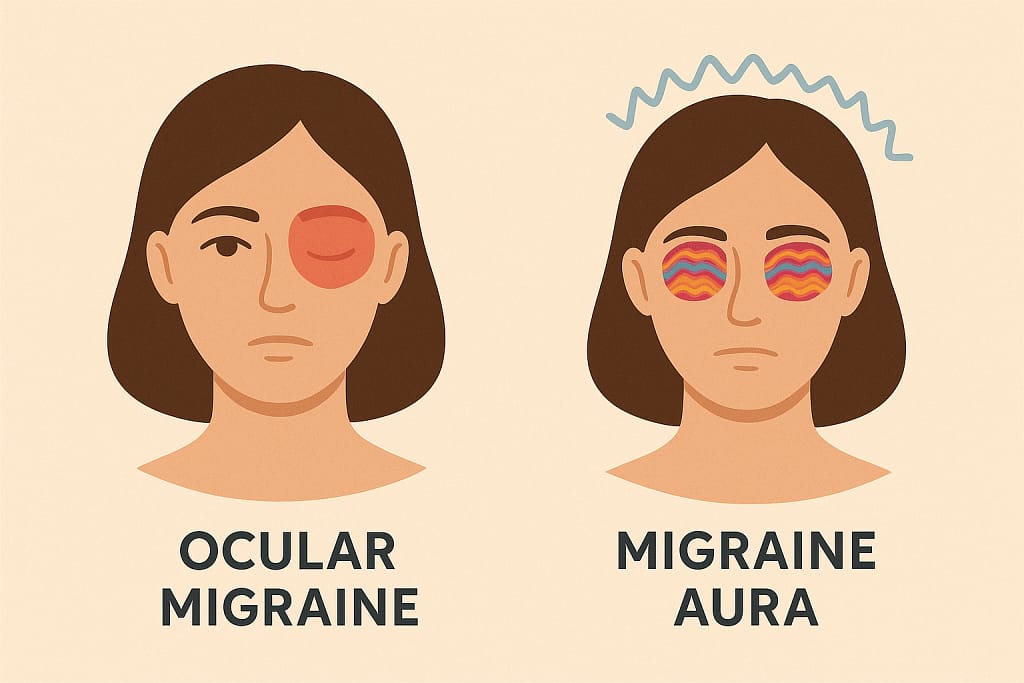
- Difference between ocular migraine (affecting one eye) and visual migraine aura (both eyes, linked to brain activity).
- Why people often confuse them with serious eye conditions (stroke, retinal detachment, glaucoma attack).
| Feature | Ocular Migraine | Retinal Detachment (Danger!) |
| Duration | 20–30 minutes | Constant / Worsening |
| Vision Loss | Temporary / Shimmering | “Curtain” falling over vision |
| Pain | Possible headache | Usually painless |
| Action | Rest in a dark room | Immediate Emergency Care |
Common Symptoms of Ocular Migraines
- Flashing or shimmering lights
- Zig-zag patterns across vision
- Blind spots (scotomas)
- Temporary blindness in one eye
- Headache (sometimes follows vision symptoms, sometimes absent)
Causes and Risk Factors
- Neurological misfiring in visual cortex or retinal blood vessels
- Genetic predisposition (family history of migraines)
- Hormonal changes (estrogen, pregnancy, birth control pills)
- Stress and anxiety (cortisol impact)
- Poor sleep, irregular meals, dehydration
💡 Did You Know?
Women are 3 times more likely to experience ocular migraines than men, largely due to hormonal fluctuations.
Triggers of Ocular Migraines
- Bright lights and screen overuse
- Certain foods (chocolate, aged cheese, red wine, processed meats)
- Caffeine withdrawal
- Strong odors and perfumes
- Weather changes (barometric pressure)
- High stress and lack of rest
Diagnosis: How Are Ocular Migraines Identified?
- Eye exam to rule out retinal detachment or vascular disease
- Neurological evaluation (EEG, MRI if needed)
- Detailed medical history (migraine patterns, family history, triggers)
According to experts at the Mayo Clinic, distinguishing between a visual aura and a retinal migraine is the most critical step in managing your symptoms.
Treatment Options
- Lifestyle Management:
- Stress reduction (meditation, yoga)
- Screen breaks (20-20-20 rule)
- Hydration & regular meals
- Medications:
- NSAIDs for pain
- Preventive migraine drugs (beta-blockers, calcium channel blockers)
- Antiepileptic drugs (topiramate)
- Supplements:
- Magnesium, riboflavin (B2), CoQ10 — shown to reduce migraine frequency
💡 Did You Know?
About 1 in 200 migraine sufferers experiences the ocular type — making it rare but very important to diagnose correctly.

Migraine Relief Ice Cap
Reduce the intensity of symptoms when ocular migraines causes symptoms strike. This wearable cap provides 360° cold therapy for instant relief.

Living with Ocular Migraines
- Keeping a migraine diary to identify triggers
- Maintaining healthy lifestyle routines
- Avoiding dangerous activities during an episode (e.g., driving)
- Seeking emergency care if symptoms persist longer than 60 minutes
⚡ Migraine Quick Check
Does your vision disturbance affect only one eye or both?
FAQ Section
Q1: What are the primary ocular migraines causes symptoms?
A1: The primary ocular migraines causes symptoms include visual disturbances like zig-zag lines, shimmering lights, or temporary blind spots. These are caused by temporary spasms in the blood vessels of the retina or the brain’s visual cortex.
Q2: Can light triggers worsen ocular migraines causes symptoms?
A2: Yes. Bright lights, screen glare, and flickering fluorescent bulbs are well-known triggers that can activate ocular migraines causes symptoms in sensitive individuals.
Q3: Is there a cure for these symptoms?
A3: While there is no “one-size-fits-all” cure, managing ocular migraines causes symptoms usually involves avoiding food triggers, reducing stress, and taking magnesium or riboflavin supplements.
Conclusion
Ocular migraines may be frightening, but they are usually temporary and manageable with proper lifestyle adjustments and treatment. By learning to recognize triggers, maintaining good overall health, and consulting an eye specialist, patients can reduce episodes and protect both their vision and quality of life.
A Note from the Founder
"I started CVT because eye health is personal to me. After losing sight in my left eye due to a childhood injury and managing high intraocular pressure for decades, I’ve dedicated my life to finding the best ways to protect the vision we have. Every piece of advice on this site is researched with that same level of care and responsibility. Thank you for being here."



