Introduction
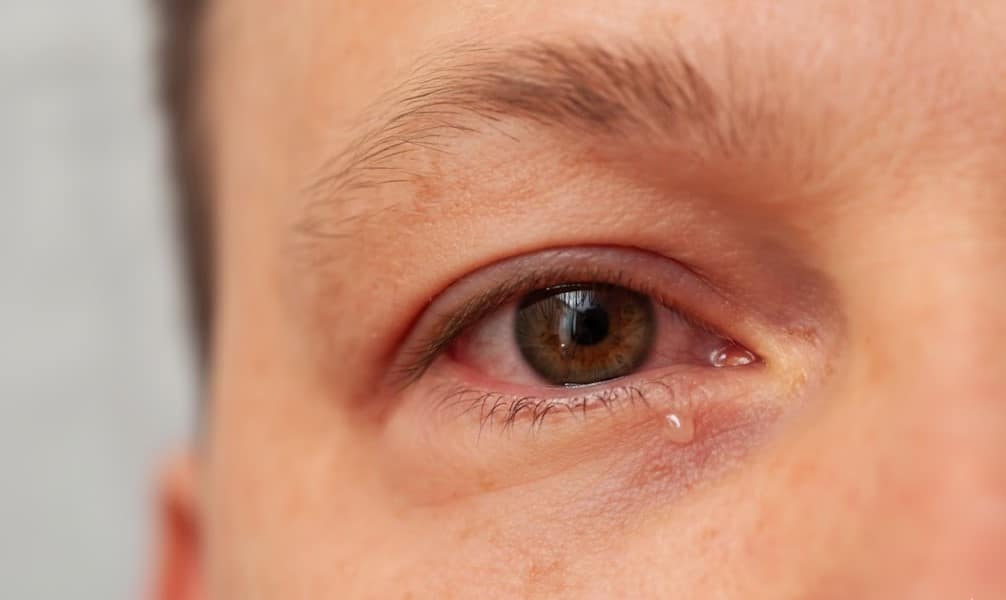
Eye inflammation, scientifically known as Uveitis, is a serious condition that affects the uvea—the middle layer of the eye responsible for supplying blood to the retina. If left untreated, this disorder can lead to pain, redness, and even permanent vision loss. While not as common as cataracts, it remains a leading cause of blindness worldwide. Understanding the triggers and available treatments is essential for protecting your sight
In this detailed guide, we will cover everything you need to know about uveitis—from what triggers it, how it is diagnosed, and what treatment options are available, to lifestyle and prevention strategies.
What is Uveitis?
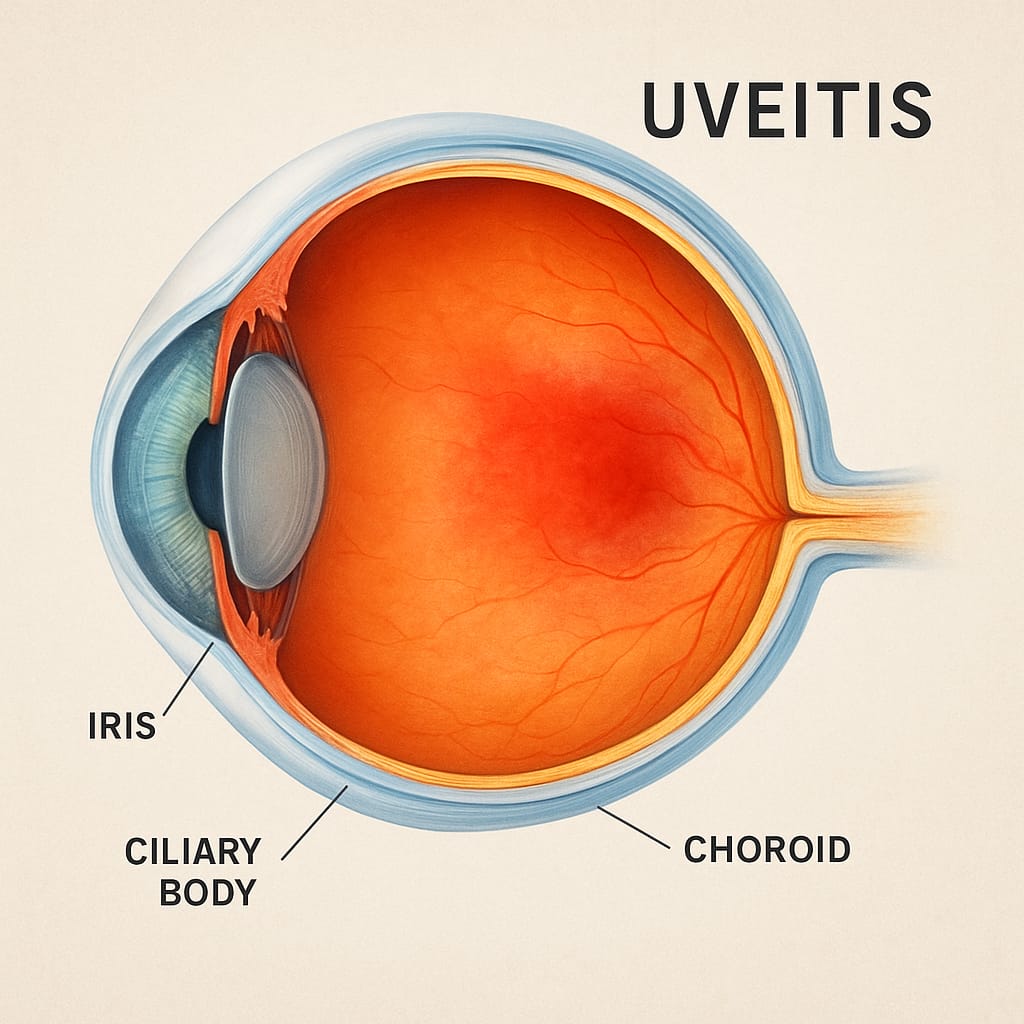
The uvea is made up of three key structures:
- Iris – the colored part of the eye.
- Ciliary body – controls lens shape and produces fluid inside the eye.
- Choroid – a layer of blood vessels that nourishes the retina.
When these structures become inflamed, the condition is referred to as uveitis. Depending on the area affected, uveitis can be categorized into:
- Anterior Uveitis (most common) – affects the iris.
- Intermediate Uveitis – inflammation in the vitreous (gel inside the eye).
- Posterior Uveitis – affects the retina and choroid.
- Panuveitis – inflammation of all parts of the uvea.
Causes and Triggers of Eye Inflammation
Uveitis can result from many factors, including:
- Autoimmune diseases
- Rheumatoid arthritis
- Ankylosing spondylitis
- Lupus
- Multiple sclerosis
- Infections
- Tuberculosis
- Syphilis
- Herpes (HSV, VZV, CMV)
- Toxoplasmosis
- Eye injuries
Trauma or surgery can trigger inflammatory responses. - Systemic diseases
Conditions such as Crohn’s disease or sarcoidosis are linked to uveitis. - Idiopathic causes
In many cases, the exact cause cannot be identified.
Common Symptoms of Eye Inflammation
Uveitis symptoms may develop suddenly or progress gradually. Common signs include:
- Eye redness
- Eye pain or tenderness
- Blurred vision
- Sensitivity to light (photophobia)
- Floaters (spots in vision)
- Reduced visual acuity
👉 If you experience these symptoms, seek medical attention immediately. Delays in treatment can lead to severe complications such as glaucoma, cataracts, or retinal damage.
Risk Factors
Certain groups are at higher risk of developing uveitis:
- People with autoimmune or systemic inflammatory conditions
- Those with a history of herpes or other eye infections
- Smokers (studies show increased risk and severity)
- Individuals with family history of eye inflammation
Diagnosis
An ophthalmologist will typically perform:
- Comprehensive eye exam – checking vision, eye pressure, and internal structures.
- Slit-lamp examination – detects inflammation inside the eye.
- Ocular imaging (OCT, fluorescein angiography) – to assess retinal involvement.
- Blood tests or chest X-rays – to identify underlying autoimmune or infectious causes.
👁️ Related Articles

Treatment Options
Treatment depends on the cause and severity of inflammation.
- Medications
- Corticosteroids (eye drops, oral, or injections) – first-line treatment.
- Immunosuppressants (methotrexate, cyclosporine, biologics) – for chronic or autoimmune-related cases.
- Antibiotics or antivirals – if infection is the cause.
- Mydriatic eye drops – help reduce pain and prevent scarring.
- Surgery
- Vitrectomy (removal of vitreous gel) may be required in severe cases.
- Surgery may also treat complications like cataracts or glaucoma caused by uveitis.
- Lifestyle and Home Care
- Regular monitoring by an ophthalmologist.
- Wearing sunglasses to reduce light sensitivity.
- Maintaining a healthy immune system through diet, sleep, and stress reduction.

Polarized UV400 Sunglasses
Crucial for Uveitis patients to manage light sensitivity and protect the inflamed uvea from UV damage.
View on Amazon →Complications of Untreated Uveitis
- Cataracts
- Glaucoma
- Retinal detachment
- Permanent vision loss
Prevention and Long-Term Management
While not all cases of uveitis are preventable, steps to reduce risk include:
- Managing autoimmune or systemic diseases with medical supervision.
- Practicing safe hygiene to reduce infection risk.
- Avoiding smoking.
- Regular eye check-ups, especially if you have a family history of autoimmune disorders.
Common Questions About Eye Inflammation
1. Is this a serious condition?
Yes. If left untreated, chronic inflammation can cause permanent vision damage or blindness. However, with prompt diagnosis, most patients maintain good sight.
2. What causes recurrent flare-ups?
Chronic autoimmune conditions, infections like herpes, or underlying systemic issues often lead to repeated episodes of Uveitis.
3. Can the inflammation go away on its own?
Mild cases may improve temporarily, but without medical intervention, the problem often returns or worsens over time.
4. How long does the recovery process take?
Depending on severity, recovery may last from a few weeks to several months. Chronic cases might require long-term management with specialized medication.
5. Can stress be a trigger?
Stress doesn’t cause the condition directly, but it can weaken the immune system and exacerbate autoimmune responses that trigger inflammation.
Conclusion
Uveitis is a potentially vision-threatening eye condition that requires early detection, accurate diagnosis, and prompt treatment. Although it can be triggered by autoimmune diseases, infections, or trauma, medical advancements now allow for effective treatment and long-term management. Protecting your eyes through regular check-ups and healthy lifestyle choices is key to preventing vision loss.
A Note from the Founder
"I started CVT because eye health is personal to me. After losing sight in my left eye due to a childhood injury and managing high intraocular pressure for decades, I’ve dedicated my life to finding the best ways to protect the vision we have. Every piece of advice on this site is researched with that same level of care and responsibility. Thank you for being here."